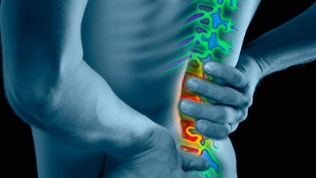
Despite the prevalence of opinion, spinal osteochondrosis is not considered part of the aging process. The elastic discs between the vertebrae are responsible for flexing and extending the back, as shock absorbers. Over time, they wear out and no longer provide full range of motion. With age, daily spinal stress and accidental injuries, including minor injuries, can damage the discs in the back and lead to osteochondrosis of the lumbar spine.
Who is affected by this disease in the lower back?

In most cases, the first symptoms of osteochondrosis of the lumbar spine occur at 11-12 years of age. The disease manifests itself vividly around the age of sixteen, but the most severe course and frequent complications occur between the ages of 15 and 20.
Children under the age of 15 rarely have severe forms of osteochondrosis, which is somehow related to the excellent condition of the musculoskeletal system in general and the spine in particular. In addition, the disease takes time to develop and, on average, five years.
Fortunately, these diseases are much easier to treat in children than in adults.
Symptoms
Reflex syndromes
- Cervicalgia- pain manifested differently in the neck (tugging, tingling, shooting), sensation of "crawling" in the cervical muscles, as well as decreased mobility and flexibility of the neck.
- Lumbagois an acute and acute pain in the lower back, which may be accompanied by numbness or swelling. Instead of the word "lumbago", the words "lumbodynia" or "lumboischialgia" can be used.
- Chest pain- pains of a different nature in the chest, shoulder blades and ribs, which are constantly present or occur during body movements.
Compression syndromes
The occurrence of pain syndrome in osteochondrosis of the lumbar spine is due to:
- Compression of root structures (radiculopathy).
- Compression of the spinal cord (myelopathy).
- Spinal cord injury due to insufficient blood supply.
- Narrowing (stenosis) of arteries and veins (vascular myeloiscemia by compression).
Methods to detect diseases
Differential diagnosis
Not every disorder can be diagnosed with a simple laboratory test. Many conditions cause similar symptoms. For example, many infections cause fever, headaches and fatigue.
Many mental disorders are caused by:

- sadness;
- concern;
- sleep problems.
The differential diagnosis identifies possible disorders that cause symptoms. This diagnosis is usually based on several tests. These tests can rule out conditions and / or determine whether you need additional tests.
Differential diagnosis is used to diagnose physical or mental health problems that cause similar symptoms.
Differential diagnosis is also commonly used in the field of psychiatry / psychology, where two different diagnoses can be made on a patient who has symptoms of various diseases. For example, a patient diagnosed with bipolar disorder may also have a differential diagnosis of borderline personality disorder, given the similarity of symptoms in both conditions.
Who is diagnosed most often?
If previously the disease was diagnosed in patients after the age of 45, today about 27% of adolescents suffer from osteochondrosis to one degree or another.
It is understandable that there is such a spread of the disease - children began to sit for a long time, including because of the computer and the Internet. Is bad? Time will tell, but the fact remains - the payment for a sedentary lifestyle is high, and osteochondrosis is far from the worst disease that can occur with that lifestyle, but it is the most common (after obesity).
How to define a disease and its degree?
First
In a normal state, the intervertebral discs are constantly regenerating, but it happens that the process slows down and a disease like 1st degree osteochondrosis occurs.
There are many reasons for this:
- obese;
- metabolic disorders;
- immunocompromised and so on.
Unfortunately, the pain instability of a certain degree of illness is influenced by the fact that many people neglect diagnosis and treatment and try to cure the pain on their own. To do this, use ointments and various tinctures. But that is the biggest mistake.
Osteochondrosis of the first lumbar spine can be cured quite easily by contacting a good specialist and performing a series of simple actions.
Grade 1 osteochondrosis is a compression of the intervertebral cartilage in the lumbar region. The main symptom at this stage is mild pain when turning or bending. Sometimes, the symptoms are more acute and of short duration due to sudden movements or significant effort.
Second
A pronounced symptom of the disease is pain in the lower back, which increases with any movement. The pain can radiate upward down the spine.
In osteochondrosis, pain can radiate to the lower extremities.
The second stage of osteochondrosis is characterized by pain that is so severe that it manifests itself even with a cough.
Additional symptoms are associated with compressed nerve endings:
- Sensitivity to lower limb changes. The main signs are: pain, numbness in the legs, high or very low sensitivity level of the skin of the lower limbs.
- Limited mobility. A person suffering from osteochondrosis (grade 2) finds that, as the disease progresses, it becomes very difficult to move.
- Increased fatigue and constant drowsiness. The patient has chronic fatigue, accompanied by irritability. This symptom is explained by the painful syndrome that constantly bothers the person.
- Troubled urination and pain in the kidney region.
Third party

By the time the patient reaches Stage 3, his posture has changed significantly. In more advanced cases, bone deformation occurs. In this phase of osteochondrosis of the lumbar spine, there is also an evident deterioration of the patient's general physical and / or mental state and a profound loss of energy.
The third stage is characterized by the appearance of narrowing of the intervertebral foramen against the background of previous changes. Hernias of the intervertebral discs are formed, the vessels in the neck and muscles are damaged. The patient has dizziness, pain in the neck.
Bedroom
The terminal stage occurs when the intervertebral disc degenerates and the disc space is destroyed. At this stage, disc thinning reaches its maximum or, even worse, disappears completely. Postural imbalance is acute and movement and flexibility are extremely limited.
Stage 4 of lumbar spine osteochondrosis is often characterized by severe pain and a high degree of physical and / or mental deterioration. There is also a permanent loss of growth and energy levels. Stage 4 is generally considered to be irreversible.
Medical consultation
Which doctor should I contact?
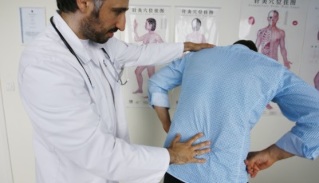
When independent treatment methods cease to have an analgesic effect, the patient begins to ask: which doctor treats osteochondrosis? The first person you can turn to to treat lumbar spine osteochondria is your local therapist. But in this situation, he plays the role of dispatcher, as he will not be able to prescribe a complete treatment - this is not his specialization.
He will probably send you to a neurologist. It is this specialist who will conduct the necessary research and help to build a treatment program. The therapist can also refer you to a vertebrologist. This doctor deals directly with diseases of the spine.
Scales and tests
Quality of life assessment
A characteristic as widespread as quality of life is especially important for a group of patients with comorbidities, as they can influence the effectiveness of treatment. This is especially important for comparing the results of various studies, economic analyzes and for understanding the problem as a whole.
Quality of life assessment methods include:
- Oswestry's quality of life questionnaire.
- Roland-Morris questionnaire.
- Stratford scale.
- Quebec Back Pain Scale - A questionnaire on how back pain affects your daily life).
Pain scales
Pain is an unpleasant sensation and an emotional experience associated with tissue damage. Its goal is to allow the body to respond and prevent further tissue damage.
Methods for assessing pain syndrome include:
- Won Korf Chronic Pain Assessment Scale.
- McGill pain questionnaire.
- Verbal pain scale.
Assessment of treatment outcome
- McNab subjective rating scale.
- Patient satisfaction scale.
- Scale of economic and functional results of Prolo.
- Scale of lumbosacral results.
- Nurik scale.
Hardware test
X-ray
X-rays provide detailed bone structures in the spine and are used to rule out back pain resulting from:
- Spondylolisthesis.
- Tumors.
- Cracks.
Calcium in the bone blocks X-ray penetration, and the image of the bones is perceived as a shadow in the film. X-rays provide excellent visibility of all the details because the bone is composed mainly of calcium. However, discs and nerve roots do not contain calcium, so X-rays do not capture images of these structures. X-rays, therefore, cannot be used to diagnose a lumbar disc herniation or other causes of a pinched nerve.
X-rays should not be done on pregnant women.
Complications and possible consequences
Complications and possible consequences of osteochondrosis of the lumbar spine include:
- Radiculopathy is a condition characterized by a disease of the nerve roots.
- Muscle weakness - common symptoms include fever, fatigue, flu-like symptoms, paraesthesia, weight loss and changes in consciousness.
- Neurogenic bladder - problems with the nerves that control the bladder and urination
- Damage to lower motor neurons.
- Raynaud's phenomenon is a condition in which spasms occur, narrowing of the capillaries of the fingers and toes.
- Pain in the neck, back, leg.
Treatment
Treatment may vary depending on the severity of your symptoms and how much they limit your daily activities.
Here are some of the treatments that your doctor may prescribe based on your level of pain:
- Non-surgical treatment- not all osteochondrosis patients require surgery. For mild to moderate pain, more conservative treatments.
- Spondylodesis- surgical intervention in the treatment of osteochondrosis.
Prevention

The prevention of osteochondrosis of the lumbar segment aims to eliminate the risk factors that lead to this disease. The elimination of factors is the main preventive measure.
Physical activity is normalized, the back muscles are strengthened, maximum load on the lower back is avoided, the development of diseases that lead to low back pain is avoided, all of this is a prophylaxis to prevent the symptoms of lumbar osteochondrosis.
Moderate exercise, lifestyle changes and good nutrition can help prevent painful and disabling symptoms.
If you notice symptoms of osteochondrosis of the lumbar spine, do not squeeze and consult a doctor immediately. A disease detected in a timely manner is easier to treat and proceeds without consequences.























